

Welcome to
Pontikas Periodontics
Welcome to Pontikas Periodontics, the office of Dr. Aristidis Pontikas, a leader in periodontal care in Phoenix, Arizona. Good periodontal health is important in achieving a healthier lifestyle, and we are committed to giving you a lifetime of healthy smiles.
Personalized Treatment
We recognize that every patient’s case is unique, and we pride ourselves on giving you the individual attention and care you deserve. From the time you walk in for your first visit, we will treat you as an individual – not a number.
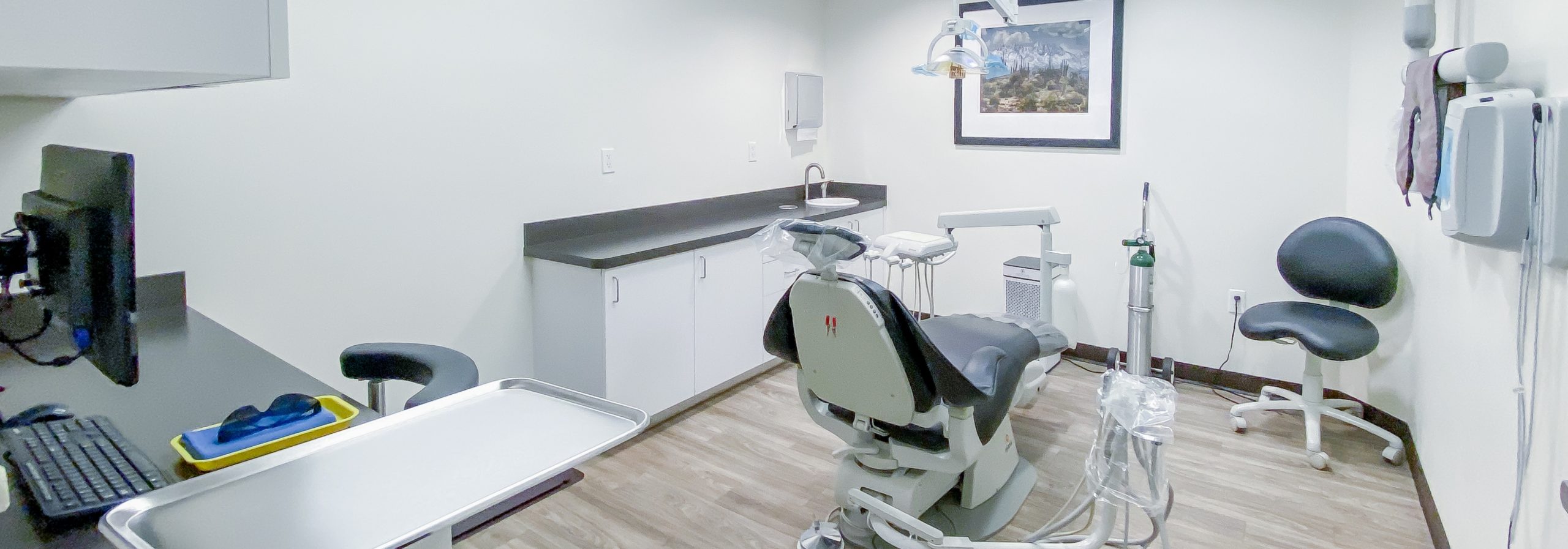
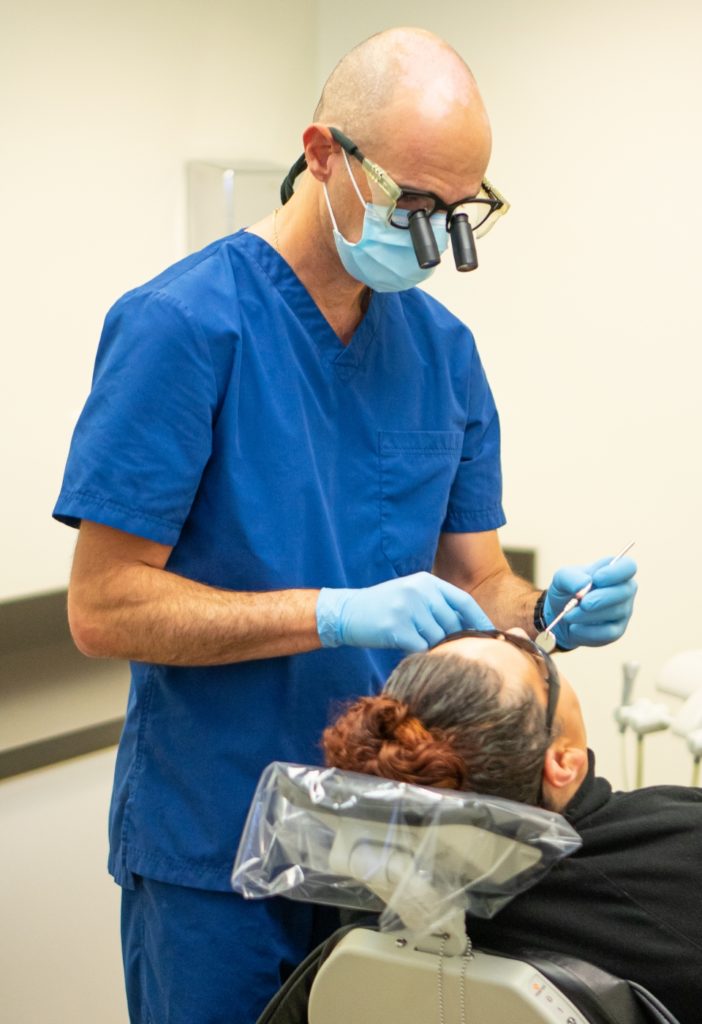

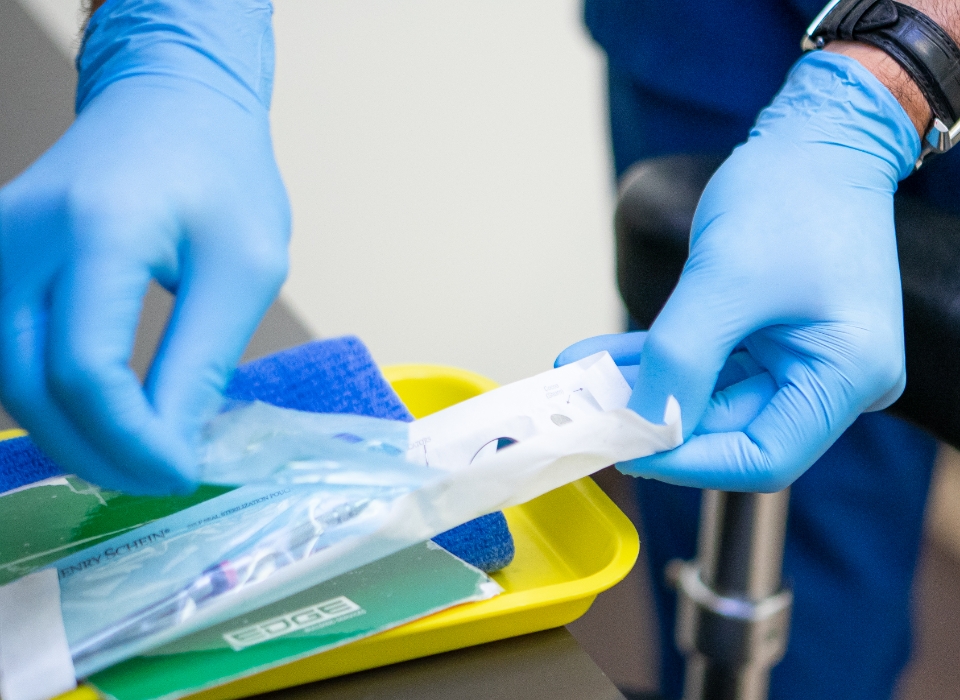
Latest Technology and Procedures
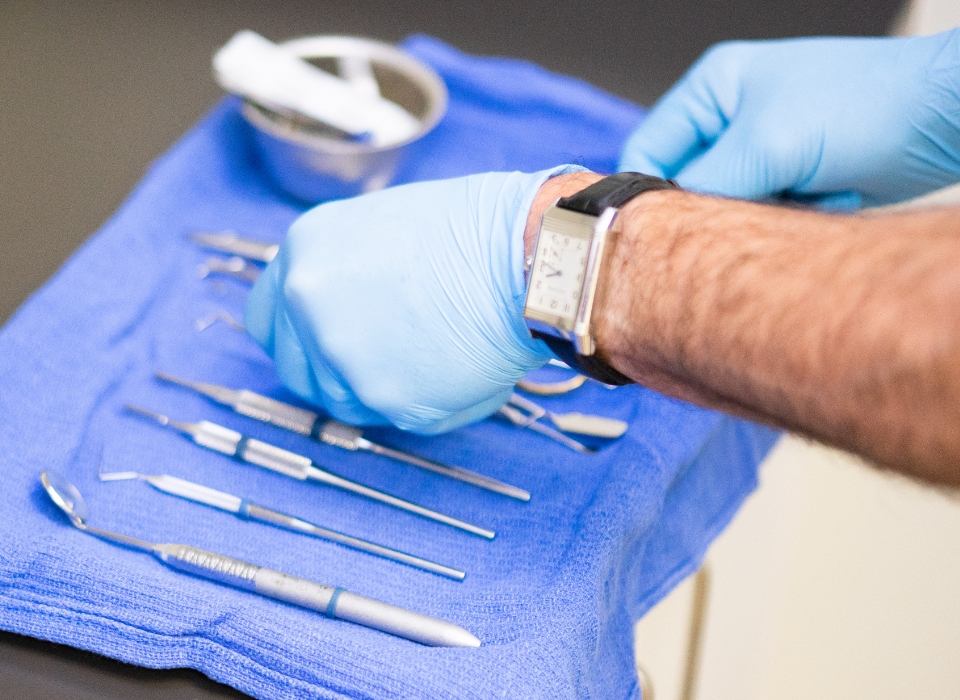
We utilize the latest technological advances in dentistry to treat all phases of periodontal disease and perform procedures such as gum grafting, crown lengthening, and dental implants using the advanced Straumann® Systems. In addition, our staff is certified in periodontal laser therapy.